Innovation & Research
Robotic Surgery &
Advanced Technologies

The Next Evolution: Digital Twin Technology
As Program Director of the HSS Digital Twin Platform, Dr. Pearle is now building what comes next: AI-driven simulations that enable true surgical personalization. Before operating on your knee, we'll operate on your digital twin; testing approaches, optimizing for YOUR sport, predicting YOUR outcome.
Skiing demands different biomechanics than tennis. Running requires different optimization than golf. For the first time, we'll be able to simulate and personalize restoration surgery for the specific activities that define your life.
Elite Surgeon. Published Researcher. Relentless Innovator.
When patients choose Dr. Pearle, they're not just getting a skilled surgeon—they're getting a dedicated physician and team whose practice continues to help shape the future of personalized orthopedic care.
Dr. Pearle brings years of masterful surgical expertise along with a relentless passion for optimizing human performance through the most up-to-date cutting-edge technological advancements. When he is not performing procedures, Dr. Pearle is researching, innovating, and speaking at conferences around the world. In short, Dr. Pearle’s contributions to robotic knee replacements have made him a true game-changing surgeon.
When Dr. Pearle performed the first robotic knee procedures over 20 years ago at HSS, the medical community took notice. What followed wasn't just adoption—it was obsessive refinement. Dr. Pearle’s surgeries literally changed the game for thousands of patients around the globe.
Dr. Pearle has not stopped pushing the limits of what’s possible with personalized orthopedic knee care. In a landmark 10-year multicenter study with the world's leading knee surgeons, the overall survivorship was 91.7%. Dr. Pearle's results were 94%, exceeding the collective average and establishing the benchmark others measure against.
This level of precision serves everyone—from world class athletes and professional performers to executives and everyday people who simply refuse to accept limitations.
The Next Evolution: Digital Twin Technology
As Program Director of the HSS Digital Twin Platform, Dr. Pearle is now building what comes next: AI-driven simulations that enable true surgical personalization. Before operating on your knee, we'll operate on your digital twin—testing approaches, optimizing for YOUR sport, predicting YOUR outcome.
Skiing demands different biomechanics than tennis. Running requires different optimization than golf. For the first time, we'll be able to simulate and personalize restoration surgery for the specific activities that define your life.
Elite Surgeon. Published Researcher. Relentless Innovator.
When patients choose Dr. Pearle, they're not just getting a skilled surgeon—they're getting a dedicated physician and team whose practice continues to architect the future of personalized orthopedic care.
Dr. Pearle brings years of masterful surgical expertise along with a relentless passion for optimizing human performance through the most up-to-date cutting-edge technological advancements. When he is not performing procedures in New York and West Palm Beach, Dr. Pearle is researching, innovating, and speaking at conferences around the world. In short, Dr. Pearle’s contributions to robotic knee replacements have made him a true game-changing surgeon.
When Dr. Pearle performed the first robotic knee procedures over 20 years ago at HSS, the medical community took notice. What followed wasn't just adoption—it was obsessive refinement. Dr. Pearle’s surgeries literally changed the game for thousands of patients around the globe.
Dr. Pearle has not stopped pushing the limits of what’s possible with personalized orthopedic knee care. In a landmark 10-year multicenter study with the world's leading knee surgeons, the overall survivorship was 91.7%. Dr. Pearle's results were 94% - exceeding the collective average and establishing the benchmark others measure against.
This level of precision serves everyone—from world class athletes and professional performers to executives and everyday people who simply refuse to accept limitations.

RIIP REPS Agility Training Program
Developed by Dr. Pearle and the Sports Medicine team at HSS, RIIP REPS (Reduce Injuries, Improve Performance) is a free app-based agility and body-control program designed to help athletes move smarter and stay healthier. Backed by over 25 years of research, these short, science-based training sessions have been shown to reduce lower-extremity injuries by up to 42% and ACL injuries by 62%.
RIIP REPS makes evidence-based injury prevention accessible to every team and athlete—no equipment, no cost, and no disruption to practice schedules. It’s part of Dr. Pearle’s mission to keep athletes on the field and in the game, safely and confidently.
RIIP REPS makes evidence-based injury prevention accessible to every team and athlete—no equipment, no cost, and no disruption to practice schedules. It’s part of Dr. Pearle’s mission to keep athletes on the field and in the game, safely and confidently.
Developed by Dr. Pearle and the Sports Medicine team at HSS, RIIP REPS (Reduce Injuries, Improve Performance) is a free app-based agility and body-control program designed to help athletes move smarter and stay healthier. Backed by over 30 years of research, these short, science-based training sessions have been shown to reduce lower-extremity injuries by up to 42% and ACL injuries by 62%.
RIIP REPS makes evidence-based injury prevention accessible to every team and athlete—no equipment, no cost, and no disruption to practice schedules. It’s part of Dr. Pearle’s mission to keep athletes on the field and in the game, safely and confidently.

The HSS Digital Twin Platform represents a major advancement in personalized orthopedic care and reflects the long-standing leadership of Dr. Andrew D. Pearle in innovation and research at Hospital for Special Surgery. Built on more than a decade of collaborative work by HSS surgeons, biomechanical engineers, and data scientists, the platform uses advanced 3D imaging, artificial intelligence, and physics-based modeling to create a virtual “digital twin” of a patient’s joint. Under the direction of Dr. Pearle, who serves as Program Director of the Digital Twin project, this technology will enable surgeons to simulate how a knee—and ultimately a hip or shoulder—moves, responds to injury, and reacts to different surgical options. These real-time, data-driven simulations enhance patient understanding while giving clinicians unprecedented precision in surgical planning.
This transformational initiative has been accelerated by a landmark $10 million gift from Lauren and Robert Steers, which includes the establishment of the Lauren and Robert Steers Chair in Orthopedic Research and Innovation, held by Dr. Pearle. The endowed chair supports the continued development and clinical expansion of the Digital Twin Platform, including early applications such as predicting the need for slope-reduction osteotomy in complex ACL revision surgery—work recently published by Dr. Pearle and colleagues in The American Journal of Sports Medicine. As the platform expands from knee applications to models of the hip and shoulder, its long-term vision is ambitious: to provide every HSS patient with a personalized digital twin care companion that integrates imaging, biomechanics, and clinical data. The Digital Twin Platform underscores Dr. Pearle’s ongoing commitment to advancing orthopedic surgery and improving patient outcomes through cutting-edge research and innovation.
The HSS Digital Twin Platform
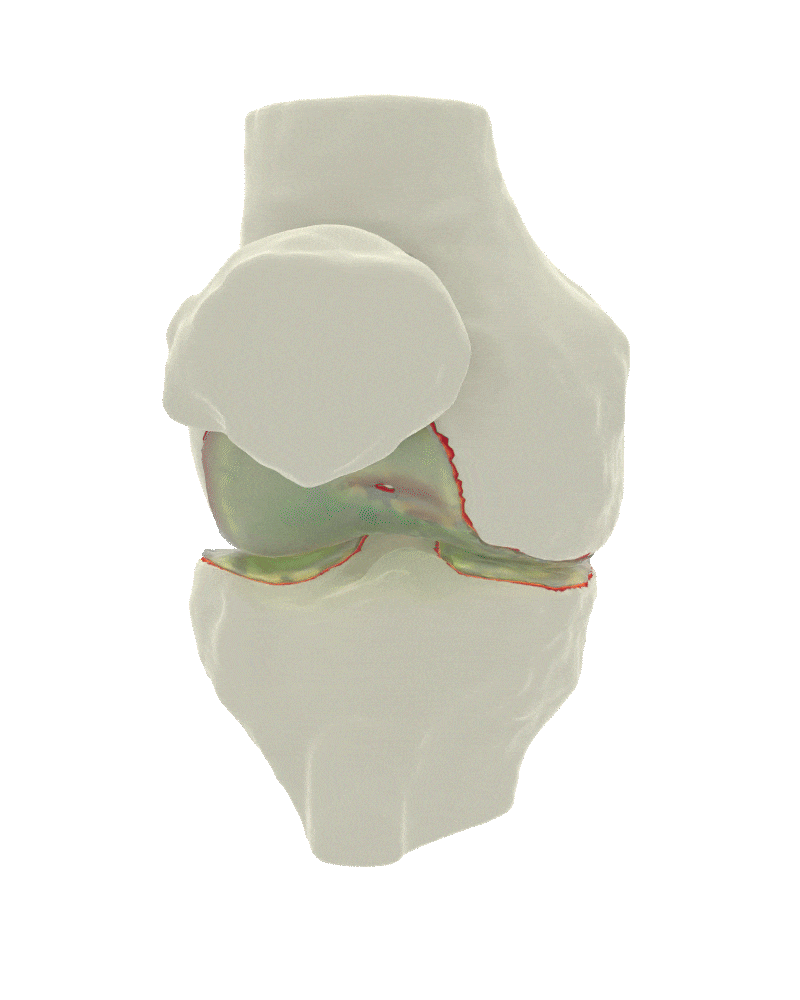
The HSS Digital Twin Platform represents a major advancement in personalized orthopedic care and reflects the long-standing leadership of Dr. Andrew D. Pearle in innovation and research at Hospital for Special Surgery. Built on more than a decade of collaborative work by HSS surgeons, biomechanical engineers, and data scientists, the platform uses advanced 3D imaging, artificial intelligence, and physics-based modeling to create a virtual “digital twin” of a patient’s joint. Under the direction of Dr. Pearle, who serves as Program Director of the Digital Twin project, this technology will enable surgeons to simulate how a knee—and ultimately a hip or shoulder—moves, responds to injury, and reacts to different surgical options. These real-time, data-driven simulations enhance patient understanding while giving clinicians unprecedented precision in surgical planning.
This transformational initiative has been accelerated by a landmark $10 million gift from Lauren and Robert Steers, which includes the establishment of the Lauren and Robert Steers Chair in Orthopedic Research and Innovation, held by Dr. Pearle. The endowed chair supports the continued development and clinical expansion of the Digital Twin Platform, including early applications such as predicting the need for slope-reduction osteotomy in complex ACL revision surgery—work recently published by Dr. Pearle and colleagues in The American Journal of Sports Medicine. As the platform expands from knee applications to models of the hip and shoulder, its long-term vision is ambitious: to provide every HSS patient with a personalized digital twin care companion that integrates imaging, biomechanics, and clinical data. The Digital Twin Platform underscores Dr. Pearle’s ongoing commitment to advancing orthopedic surgery and improving patient outcomes through cutting-edge research and innovation.
The HSS Digital Twin Platform
Publication & Research Highlights
Dr. Pearle has authored more than 250 publications in leading orthopedic journals, including The American Journal of Sports Medicine, The Journal of Arthroplasty, and The Journal of Bone and Joint Surgery. His research has helped shape modern techniques in ACL reconstruction, knee biomechanics, and robotic joint replacement—improving surgical precision, safety, and recovery for patients worldwide.
Through this ongoing work, Dr. Pearle continues to advance orthopedic innovation and ensure every patient benefits from the latest scientific insight.
Here are select publications from Dr. Pearle’s research, offering insight into the scientific progress behind today’s orthopedic techniques.
Phone: (212) 774-2878
Fax: (212) 774-2798
Hours: Mon- Fri: 9:00a - 12:30p and 1:30p - 4:00p
New York - Manhattan
Hospital for Special Surgery
The Pavilion
541 East 71st St., 1st floor
New York, NY 10021
New York - Westchester
HSS Westchester
1133 Westchester Ave, 2nd floor
Building B
White Plains, NY 10605
© 2025 Andrew Pearle MD. Orthopedic Surgeon New York NY
About / Specialties / Patient Resources / Innovation & Research / Contact / Privacy Policy
Privacy Policy












